Warning Signs of Iron Deficiency Anemia You Shouldn’t Ignore
Understanding Iron Deficiency Anemia: Symptoms, Causes, and Recovery
Iron deficiency anemia is the most common nutritional disorder in the world, affecting more than 1.2 billion people globally. It occurs when your body doesn’t have enough iron to produce hemoglobin, the protein in red blood cells that enables them to carry oxygen to your tissues.
Without enough iron, your body effectively runs on “low battery.” This guide explores everything you need to know about identifying, treating, and preventing this condition.
What is Iron Deficiency Anemia?
In simple terms, iron deficiency anemia is a condition where the blood lacks adequate healthy red blood cells. Iron is the primary building block for hemoglobin. If you are iron-deficient, your heart has to work harder to pump oxygen through your system, leading to the hallmark symptom of the condition: exhaustion.
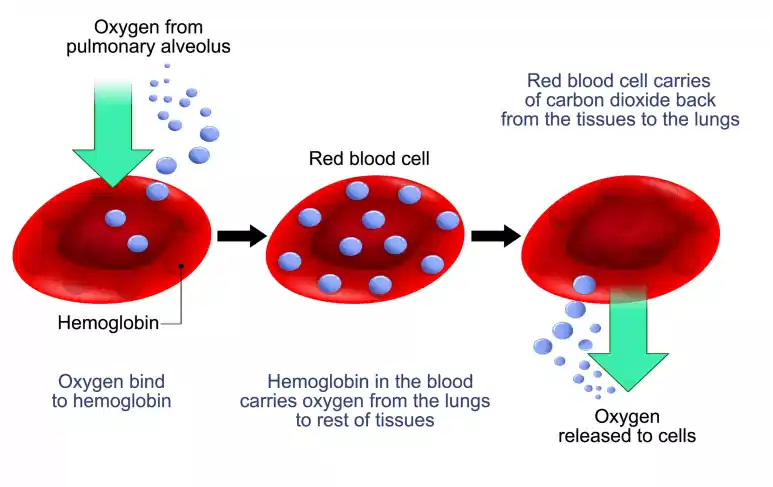
The Role of Red Blood Cells
Your body uses iron to make hemoglobin. Hemoglobin gives red blood cells their color and allows them to pick up oxygen in the lungs and drop it off throughout the body. When iron levels drop, the production of these cells slows down, and the cells that are produced are often smaller and paler than normal.
Common Symptoms to Watch For:
The symptoms of iron deficiency anemia can be so mild at first that they go unnoticed. However, as the body becomes more deficient, the signs intensify.
-
Extreme Fatigue: Feeling tired even after a full night’s sleep.
-
Pale Skin: A loss of healthy color in the skin, inner eyelids, or nail beds.
-
Shortness of Breath: Feeling winded doing basic tasks like climbing stairs.
-
Cold Hands and Feet: Poor circulation due to low oxygen levels.
-
Pica: Unusual cravings for non-nutritive substances like ice, dirt, or starch.
-
Brittle Nails or Swollen Tongue: Physical changes in the extremities and mouth.
Major Causes of Iron Deficiency
Understanding why you are low on iron is the first step toward a permanent fix. There are generally four main reasons:
1. Inadequate Dietary Intake
Your body regularly gets iron from the food you eat. If you consume too little iron over a long period, your body’s stores become depleted. This is common in strictly vegan or vegetarian diets if not carefully managed.
2. Blood Loss
Iron is stored within red blood cells. Therefore, if you lose blood, you lose iron.
-
Women: Heavy menstrual periods are a leading cause of anemia.
-
Internal Bleeding: Peptic ulcers, hiatal hernias, or colorectal cancer can cause slow, chronic blood loss.
3. Inability to Absorb Iron
Even if you eat enough iron, your body might not be absorbing it. Conditions like Celiac disease or surgeries like gastric bypass can interfere with the small intestine’s ability to pull nutrients from digested food.
4. Pregnancy
During pregnancy, iron stores need to serve the mother’s increased blood volume as well as provide hemoglobin for the growing fetus.
Diagnosis: How Doctors Check Your Levels
If you suspect you have anemia, a simple blood test called a Complete Blood Count (CBC) is the gold standard. Doctors look at several specific markers:
| Marker | What it Measures |
| Hemoglobin | The oxygen-carrying protein level. |
| Hematocrit | The percentage of your blood volume made of red cells. |
| Ferritin | A protein that helps store iron in your body (shows your “backup” supply). |
| Serum Iron | The amount of iron currently circulating in your blood. |
Treatment and Diet: Boosting Your Iron
Treatment usually involves a two-pronged approach: increasing iron intake and addressing the underlying cause of blood loss or malabsorption.
Top Iron-Rich Foods
There are two types of dietary iron: Heme (from animal products) and Non-Heme (from plant sources). Heme iron is absorbed more efficiently by the body.
-
Heme Sources: Red meat (beef, lamb), poultry, and seafood.
-
Non-Heme Sources: Spinach, lentils, beans, fortified cereals, and pumpkin seeds.
Pro Tip: To maximize absorption of non-heme iron, pair it with Vitamin C. Drinking orange juice with your spinach salad can significantly increase the iron your body keeps!
Iron Supplements
If diet alone isn’t enough, your doctor may prescribe iron tablets.
-
Take on an empty stomach if possible for better absorption.
-
Avoid antacids or milk at the same time, as calcium can block iron absorption.
-
Expect side effects: Iron pills can cause constipation or dark-colored stools.
Read More:
Importance of Vitamin D Drops for Infants
When to See a Professional
Iron deficiency anemia isn’t something to self-diagnose. Taking excess iron supplements when you don’t need them can be dangerous, as iron overload can damage your liver and heart.
If you are experiencing persistent, unexplained fatigue, schedule a blood test. Most people begin to feel significantly better within a few weeks of starting treatment, though it can take several months to fully replenish your body’s iron “vaults.”
Summary Checklist for Prevention
-
Eat a balanced diet rich in leafy greens and lean proteins.
-
Pair iron with Vitamin C (strawberries, citrus, bell peppers).
-
Monitor heavy cycles and discuss them with a gynecologist.
-
Get regular checkups if you are a frequent blood donor or have digestive issues.
By staying proactive and listening to your body’s signals, you can keep your energy levels high and your blood healthy.
Frequently Asked Questions (FAQ)
1. How long does it take to recover from iron deficiency anemia?
Most people begin to feel an increase in energy levels within 2 to 4 weeks of starting iron supplementation. However, it typically takes 3 to 6 months of consistent treatment to fully replenish your body’s iron stores (ferritin levels) and prevent a relapse.
2. Can I fix iron deficiency with diet alone?
It depends on the severity. If your iron stores are significantly depleted, diet alone is often insufficient because the body can only absorb a small percentage of dietary iron at a time. In these cases, doctors usually recommend a combination of iron-rich foods and high-dose supplements to bridge the gap quickly.
3. Why does iron cause stomach upset or constipation?
Iron supplements are known to be tough on the digestive tract. They can irritate the stomach lining or alter gut bacteria, leading to nausea or constipation. To mitigate this, try taking a “gentle” iron formula (like iron bisglycinate) or taking your supplement with a small amount of food, though this may slightly reduce absorption.
4. Is it possible to have too much iron?
Yes. Unlike some vitamins that you pee out when you have an excess, iron is stored in your organs. Hemochromatosis is a condition where too much iron builds up in the body, which can damage the liver, heart, and pancreas. Never start high-dose iron therapy without a blood test confirming a deficiency.
5. Does drinking tea or coffee affect iron levels?
Yes, specifically when consumed with meals. Tea and coffee contain tannins and polyphenols that bind to iron (especially non-heme iron from plants) and prevent it from being absorbed. It is best to wait at least one hour after eating before enjoying your caffeine.
6. Can iron deficiency cause hair loss?
Yes. When your body is low on iron, it prioritizes sending oxygen to vital organs (like your heart and brain) and “borrows” iron from non-essential storage, like your hair follicles. This can lead to thinning or shedding, which usually reverses once iron levels are restored.